Pain does not kill, but pain pills do
Dr. Beth Goldman
| 4 min read
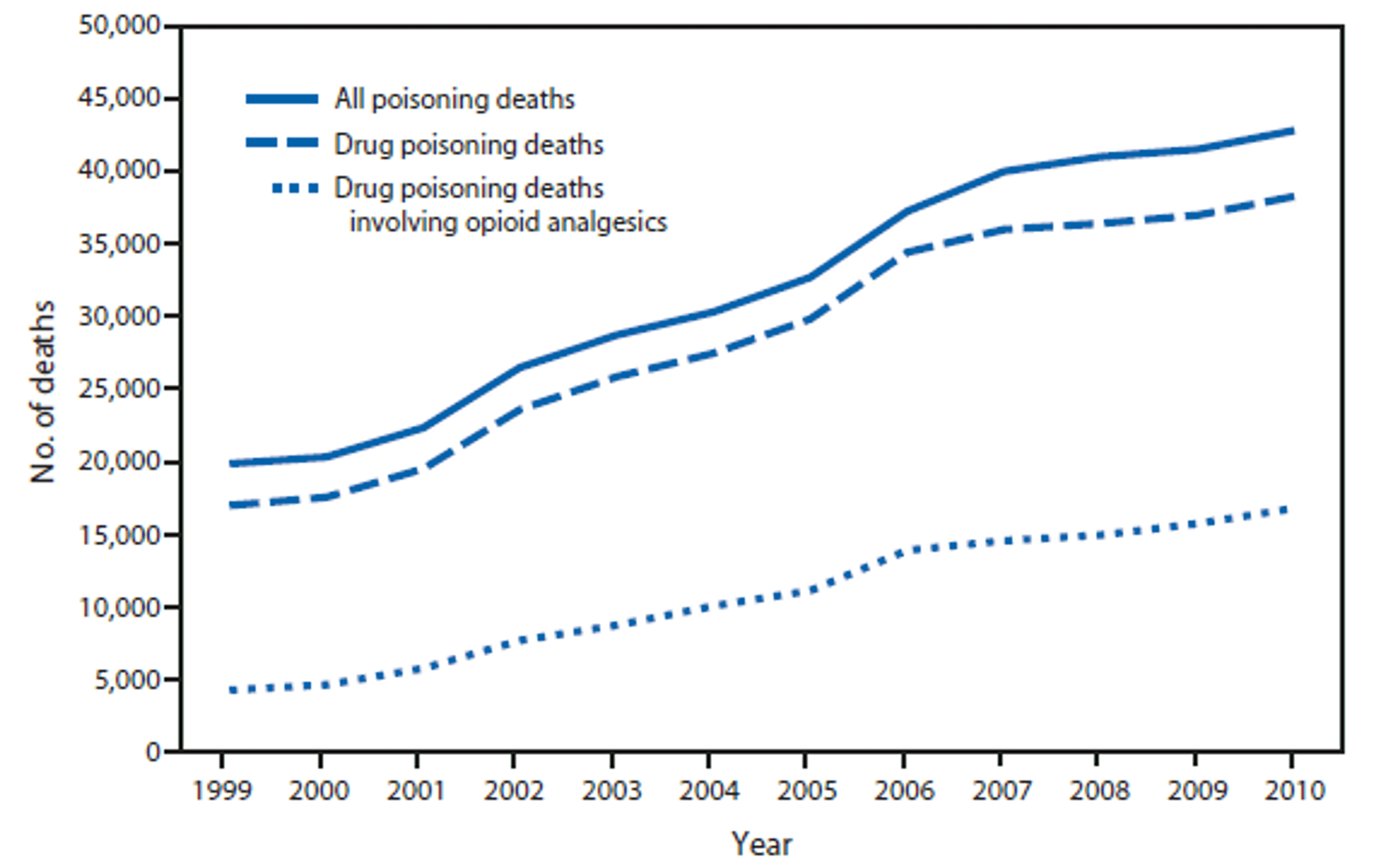
From CDC: QuickStats: Number of Deaths From Poisoning, Drug Poisoning, and Drug Poisoning Involving Opioid Analgesics — United States, 1999–2010
2008 is the first year that drug poisoning replaced automobile accidents as the leading cause of accidental death in the United States. A major reason for this is that doctors are writing more prescriptions for narcotic pain-pills (opiate analgesics) than ever before. Between 1999 to 2010, the number of US drug poisoning deaths that involved narcotics (such as oxycodone — aka Oxycontin and others, methadone and hydrocodone – aka Vicodin, Norco, Lorcet, Lortab ) more than quadrupled, accounting for over 40 percent of all drug poisoning deaths and 39% of the total poisoning deaths in 2010. This is in contrast to 1999 when these drugs were responsible for only 24% of all drug poisoning death and 20% of total poisoning deaths.
Painkiller abuse is rising in the United States and is linked to increased addiction and deaths. These are the most abused drugs and the vast majority — (71%) — of the world’s oxycodone, and a stunning 99% of the world’s hydrocodone — is consumed in the United States. The rest of the world’s doctors simply do not treat pain in the same fashion as American physicians. As a result we have seen an over three-fold increase in drug treatment admissions related to painkiller abuse between 1995 and 2005. Deaths from painkiller abuse are more than four times the deaths caused by the street drugs heroin and cocaine combined!
Part of the reason why painkillers have become abused so much is because they are easily available. Another cause is the way physicians respond to patients’ complaints of pain. Not so long ago, doctors and nurses were so afraid that patients would become addicted that they usually waited for them to experience severe pain before prescribing narcotics, and they often did not prescribe high enough doses often enough to prevent pain. This was particularly a problem for patients with chronic pain for conditions like cancer or severe osteoarthritis.
That began to change in 1996 when James Campbell, president of the American Pain Society stated ,” if pain were assessed with the same zeal as other vital signs are, it would have a much better chance of being treated properly.” This society trademarked the phrase “Pain: the fifth vital sign” in order to foster the routine gathering of information about pain. The VA enacted a national strategy in 1998, which required providers to document the patient’s report of pain on a 0-10 scale. This practice eventually became standard in most health-care settings. Over a decade later, the results have been mixed. In one study, it was assessed that there was no difference in the quality of clinicians’ pain management before and after making pain the 5th vital sign. In another study, patient satisfaction scores increased, but so did adverse reactions to narcotics.
So what happened? Many people believe that measuring pain as the fifth vital signs sent the wrong message to doctors, nurses and patients. Pain, rather than being viewed as a normal part of the healing process, became viewed a thing that should be abolished completely, as if it were a disease in and of itself. And since narcotics provided a rather reliable “quick fix” for pain, they were prescribed rather indiscriminately.
Narcotics do have their place. Patients who have terminal illness such as cancer with intractable pain should be given opiates, and plenty of them, as should other patients whose pain is not likely to go away. However those patients with conditions, such as lower back pain or post-operative pain, in which the pain is likely to go away in a relatively short time, should be either not be prescribed these agents, or should only receive enough for a few days. Patients with lower back pain should not be leaving emergency rooms or doctors’ offices with a bottle of thirty Vicodins with three refills.
What can you do if you have a problem with pain? I urge you discuss it frankly with your doctor or the emergency room doctor. Ask the doctor what to expect in the way of pain. Will my pain get better over time? How long will it take? What things can I do to help with the pain besides taking medication? How well will non-narcotic medications work for my pain? Please don’t just let the doctor give you carte blanche if he does prescribe a narcotic. Ask for a few pills, and do not get any refills. Try not to take these pills for more than a couple of days. Expect to have some pain as you heal. Although you may have to put up with some pain at first, you will not end up with the bigger problem of becoming accidentally dependent on the pain medication. (And by the way, many people who become addicted to opiates develop a reduced tolerance for ANY kind of pain – called opioid induced hyperalgesia.)
Please be careful and don’t become a statistic. Remember, pain doesn’t kill people. Pain pills do.
Photo credit: Centers for Disease Control and Prevention





